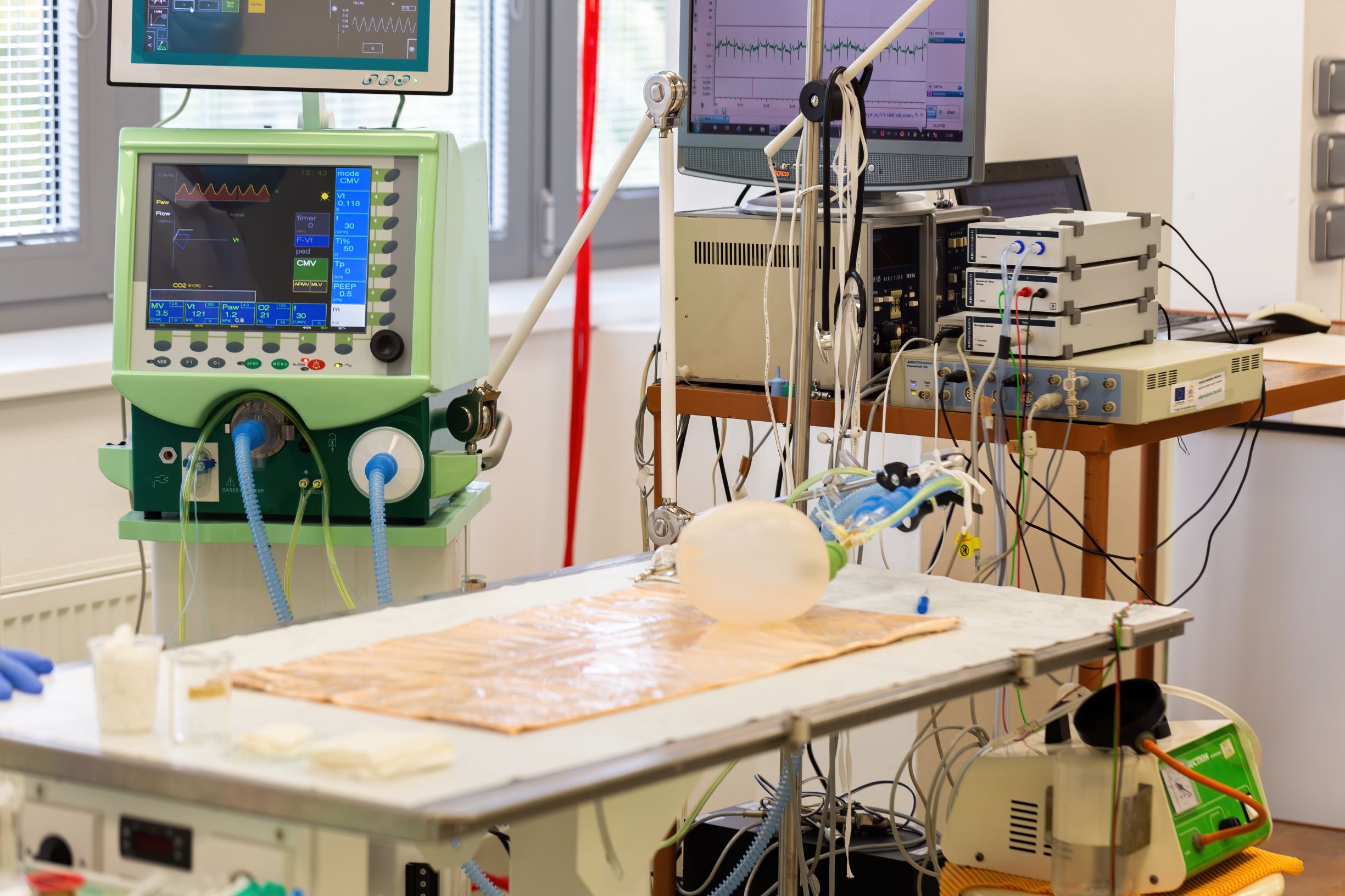
The most sophisticated patient monitors in the hospital setting are limited to three areas: the intensive care units (ICU), the operating room (OR), and post-anesthetic care units (PACU). These areas are managed 24/7 by critical care doctors and anesthesiologists to monitor beat-to-beat variability on patient’s vital signs.
COVID-19 brought so much devastation in bringing unprecedented pressure on the healthcare system. Hospitals cannot simply afford to admit low-risk patients to ICUs just for monitoring purposes. Step-down wards were then created for patients who have been recently admitted but deemed can be monitored at home until symptoms improve.
Tech companies responded to this demand to help reduce workload fatigue in ICU step-downs. Desperate to free up beds for the sickest COVID-19 patients, hospitals are considering using new technologies such as remote patient monitoring to continue care for patients from their homes.
Remote patient monitoring has been around for years, but its adaptation only became widespread when the COVID-19 pandemic began. In its early implementation, the limited reimbursement opportunities were one of the major drawbacks of the use of RPM. Still, lawmakers are continuously advancing reforms to promote advanced health through telemedicine and remote patient monitoring.
The pandemic brought telemedicine in a new light, reducing hospital readmissions and unnecessary trips to the clinics. While health care providers can benefit from lesser exposure to COVID-19, ICU step-downs can benefit from RPM thru the following:
More patient mobility
While monitors in ICUs are connected to wires 24/7, one of the big advantages of RPM is its wireless medical sensors that allow patient mobility. This innovation lessens false alarms due to patient movement.
General hospital wards usually check vital signs every 4 to 8 hours, and most of the day, patients go unmonitored. With RPM, a non-invasive ward monitoring can be more automated, which decreases the workload of our health care providers.
More smartphone versatility
Smartphones are handier for both health care providers and patients. Incorporating RPM in smartphones enables a higher level of health care surveillance among patients. DrKumo, a leader in next-gen RPM connected health technology, provides wireless medical sensors where a simple mobile app can acquire patients’ health data.
With its wireless feature, RPM benefits critical care doctors to monitor patients from an offsite location. Advanced patient engagement tools help with early detection and allow health care providers to intervene quickly when critical changes occur. Optimized interventions lead to a shortened chain of command between health care providers.
More collaboration with AI
Data acquired from medical sensors, such as ECG, heart rate, oxygen saturation, and temperature, helps develop AI-based algorithms to predict early symptoms and severity of the disease. AI is a game-changer with regards to patient monitoring. Increasing levels of patient engagement are associated with better outcomes in RPM. With basic monitoring, no one needs to die.
Some health care providers may have lesser reliance on the progressing digital health care. Some providers would see it as barriers, afraid they might lose their clinical skills with less interpersonal communication. Trusting technology takes a big step for these health care models to work. Proper education and training may help broaden health care into brand new horizons and may put a high level of patient monitoring.
The flexibility of telehealth among hospitals
While the vaccines for COVID-19 are still on the rollout, deaths and numbers of infected patients continue. The American Hospital Association urged HHS and CMS to provide hospitals with the flexibility for telehealth treatment to continue beyond the pandemic to enable the most efficient and effective provision of telehealth to their patient. Their recommendations include:
- expanding the list of Medicare telehealth services to include services added during the COVID-19 pandemic;
- allowing virtual check-ins and e-visits to be used for new and established patients;
- allowing remote patient monitoring to be used for new and established patients, and acute and chronic conditions; and
- allowing direct supervision to be provided using real-time, interactive audio and video technology.
CDC continues to investigate health effects, both short-term and long-term, affecting even previously asymptomatic COVID-19 patients. Previously admitted patients can be continuously monitored at home and checked for the following symptoms: shortness of breath, lung function abnormalities, intermittent fever, or chest pain. Long-term significance is unknown but can last for weeks or months after recovery from acute illness.
In conclusion, remote patient monitoring provides great assistance to health care providers and can lessen hospital work fatigue by giving earlier ICU step-downs. It can even benefit in rural hospitals, where there is a shortage of critical care doctors. Patient and healthcare provider training might be the key determining factor of these innovative health care models’ success. With collaboration with lawmakers, tech companies, and hospitals, health care providers will be able to provide patient care with the right tools.
Reference: